Overnight Oximetry to Test for Low Oxygen Levels
Sleep-related breathing disorders, specifically obstructive sleep apnea, is a common condition that regularly goes unrecognized. Approximately three to seven percent of the general population suffers from sleep apnea, with 93 percent of women and 82 percent of men remaining undiagnosed. If obstructive sleep apnea goes undiagnosed and untreated, it can result in serious life-threatening conditions and events such as high blood pressure, heart disease, stroke, diabetes, depression, and automobile accidents. For these reasons, it is essential to screen and test for obstructive sleep apnea with overnight oximetry for high-risk individuals, or individuals showing signs or symptoms that are affecting daily activities.
Obstructive sleep apnea is a condition that causes the airway to repeatedly become blocked, preventing air from reaching the lungs. After falling asleep, the muscles in the throat relax and collapse into the upper airway, limiting the amount of air that can pass through and ultimately depriving the body of much-needed oxygen. When this happens, the brain begins to feel the effects of oxygen deprivation and alerts the body to wake up and breathe. This usually results in a snore or choking noise that can partially or fully awaken the individual. If the individual is not fully awakened, they may be unaware of how many times this occurs each night or that there is a problem. These episodes can occur several times a night and last 10 seconds or longer, depending on the severity of the condition. Because sleep apnea causes fragmented sleep. It disturbs the natural sleep cycle, leading to daytime drowsiness, fatigue, difficulty concentrating, and headaches, and can contribute to other long-term health consequences.
Currently, diagnosing obstructive sleep apnea, or OSA requires an in-lab overnight polysomnographic test or an at-home sleep test. While an in-lab test is still the most accurate in diagnosing OSA, it is time-consuming and expensive. Also, a sleep lab may not provide the most comfortable environment for the individual due to the artificial environment and the inability to perform their typical bedtime routine. While some may not want to go through these extensive tests immediately, a simple screening tool can be used to monitor blood oxygen levels throughout the night to determine if there is a significant risk of sleep apnea. An overnight pulse oximetry test is a less invasive, straightforward study of oxygen saturation, as well as heart rate. Both oxygen saturation and heart rate will indicate whether an “apnea” event occurs at a given time throughout the night.
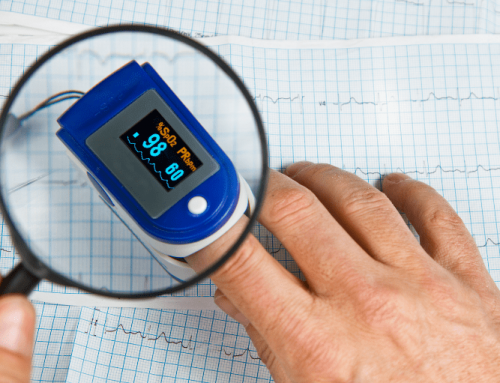
A pulse oximeter is a clip placed on a finger and connects to a small device that continuously records data overnight. The pulse oximeter emits an infrared light that shines through the finger and detects the amount of light reflected off the gases in the blood, indicating the percentage of blood that is bound to oxygen. As the blood is pumped through the arteries, the oxygen content will change, and a new reading will be produced. These readings are generated into a graph that indicates whether oxygen saturation levels fluctuate and how the heart rate responds to the oxygen change. Normal values of oxygen saturation range from 95 to 100 percent. If oxygen levels drop below normal, it is referred to as a desaturation event. If an increase in heart rate accompanies a desaturation event, it may suggest sleep apnea. The increase in heart rate is due to a spike in the stress hormone cortisol. When these events occur multiple times an hour, cortisol levels remain high, which can negatively affect the heart over time. The severity of sleep apnea is diagnosed based on how many desaturations occur per hour. In certain conditions, such as COPD, oxygen levels will consistently remain between 88 and 92 percent. This can be normal, but a physician must be aware of this underlying condition and the individual’s normal oxygen saturation levels.
While overnight pulse oximetry does not provide enough information to fully diagnose sleep apnea, it helps determine whether additional testing is necessary. This is a great option for people who do not have the time or money to undergo a full in-lab sleep study. Pulse oximetry is also valuable in determining if supplemental oxygen is necessary or if current treatments are effective. Overnight pulse oximetry is a non-invasive, simple, self-administered test that can be performed from the comfort of your own bed. If you struggle with snoring that disrupts you or your partner’s sleep, or if you have a history of smoking, chronic bronchitis, pneumonia, or asthma, you may benefit from oximetry testing. Start with Vitalistics’ pre-screening questionnaire and bring the results to your physician. Your physician will order the test, and Vitalistics will send the device directly to your home. Perform the test when it is convenient for you, and you can follow your usual nighttime routine. After performing the test, simply return the device to Vitalistics, and we will send the results directly to your physician, who will determine the best treatment option. Don’t continue to suffer from disrupted sleep. Vitalistics is here to help!