Determine Your Oxygen Levels With Oximetry Testing
Pulse oximetry has become increasingly useful in checking the oxygen levels in the blood. Prior to the invention of the pulse oximeter in 1972, the only way to detect oxygen content was through an invasive, painful, arterial blood draw. Luckily, the pulse oximeter became commercially available in the 1980s, which provided patients with a simple, non-invasive way to measure oxygen saturation. Originally, pulse oximetry was only used in the operating room to monitor patients that were under sedation, but as pulse oximetry evolved and improved, its use quickly spread to other areas of medicine and at-home use. Since its increased use in health care, oxygen saturation has become the fifth vital sign and is essential in diagnosing certain medical conditions.
The purpose of pulse oximetry is to determine how well oxygen is being transported throughout the body. Oxygen is carried throughout the body by a protein called hemoglobin located in red blood cells. The blood coming from the heart travels through the arteries and delivers nutrients including oxygen to organs, so they can continue to function normally. Without oxygen, the vital organs start to suffer, particularly the heart and brain, and a condition called hypoxemia occurs. Some conditions that can interfere with the body’s ability to deliver normal amounts of oxygen include COPD, asthma, pneumonia, lung cancer, anemia, sleep apnea, heart disease, heart failure, and congenital heart defects.
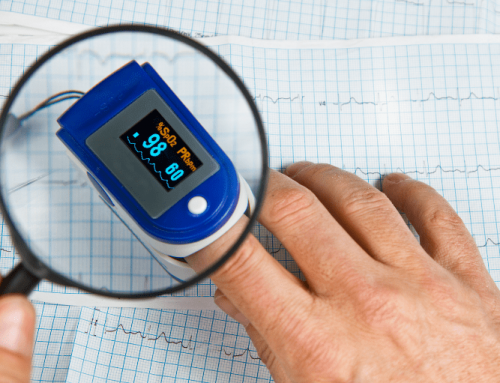
A pulse oximeter detects oxygen content by positioning a clip on a finger, toe, or earlobe. The device emits a red and infrared light that shines through the finger to the other side of the device. As both beams of light shine through the finger, the oxygenated blood absorbs the infrared light, allowing more red light to pass through to the sensor on the other side of the device. Deoxygenated blood absorbs the red light, which allows the infrared light to pass through. The amount of light that the sensor detects is measured and gives a ratio of red light to infrared light, which is then converted into an oxygen saturation percentage, or SpO2. Normal readings are 95 to 100 percent. Any readings under 90 percent are considered low and can suggest hypoxemia.
There are several circumstances in which pulse oximetry can be used. For example:
- Assess how certain lung medications are working.
- Evaluate the need for supplemental oxygen or how well a current treatment is working.
- Monitor oxygen levels during or after surgical procedures.
- Evaluate ventilator effectiveness.
- Assess one’s ability to tolerate physical activity.
Pulse oximetry is particularly useful in screening for sleep apnea. The pulse oximeter is worn overnight and continuously records oxygen saturation and heart rate. If an event occurs where oxygen content drops and heart rate increases, it is identified as an apnea event. If these events occur several times an hour and last 10 seconds or longer, sleep apnea may be the cause. Pulse oximetry can also be used to determine the severity of sleep apnea by evaluating how many apnea events occur per hour. If the overnight pulse oximetry test shows a significant risk for sleep apnea, then a home sleep test is necessary for proper diagnosis.
If oxygen saturation is low, there are certain lifestyle changes, in addition to medical interventions, that can help increase blood oxygen levels. It can be as easy as improving your daily habits like not smoking and avoiding areas where others are smoking, maintaining a healthy diet, and exercising regularly to improve heart and lung function. These practices are beneficial to living an overall healthy life, but medical intervention may be required if hypoxemia is severe. Supplemental oxygen has the most significant and direct impact in treating hypoxemia and raising oxygen saturation quickly. Oxygen use may be necessary 24/7 or on an as-needed basis depending on the diagnosis or what your physician recommends.
Pulse oximetry has become the standard of care in many areas of healthcare. It is an easy, non-invasive, and quick way to provide an early indication of heart or lung problems that can affect oxygen levels in the bloodstream. Some symptoms that may suggest low oxygen levels are headaches, shortness of breath, fast heartbeat, coughing, wheezing, confusion, blue skin, fingernails, or lips. If you notice any of these symptoms, it is important to discuss them with your physician to find the underlying cause. However, if you suspect you could be suffering from obstructive sleep apnea or have noticed loud snoring, excessive daytime sleepiness, abrupt nighttime wakings, morning headaches, or sore throat, let Vitalistics help! Start with our online sleep assessment to determine if you have any risk factors for sleep apnea. Then, consult with your physician about using Vitalistics’ at home overnight oximetry testing to screen for obstructive sleep apnea. Low oxygen levels can lead to potentially serious health conditions; therefore, it is important to be aware of oxygen content so the organs can maintain proper function and you can live an active, healthy life.