Making Diagnosis Easier With Pulse Oximetry
Sleep apnea is one of the most common sleep disorders, affecting nearly 22 million Americans. However, diagnosis of this condition remains low, with 80 percent of moderate to severe cases being undiagnosed. What’s unsettling about this is untreated obstructive sleep apnea can lead to cardiovascular problems, including high blood pressure, heart failure, atrial fibrillation, and stroke. In addition to cardiovascular conditions, sleep apnea can also contribute to type 2 diabetes, and automobile accidents due to drowsy drivers. It can even play a role in mental health, leading to depression. But why does sleep apnea continue to be missed in the majority of the population and remain undiagnosed?
Obstructive sleep apnea is a condition in which breathing is hindered or stops completely for a duration of time throughout the night. These episodes last 10 seconds or longer and occur five to 30, or more, times an hour. These breathing disturbances occur because the soft tissues in the back of the throat and the tongue collapse against the back of the throat while asleep, closing off the airway. When the brain detects the pause in breathing, it alerts the sleeper and causes them to wake up suddenly to resume breathing, resulting in fragmented, low quality sleep. Some common symptoms associated with sleep apnea are loud snoring, abrupt awakenings, excessive daytime sleepiness, dry mouth or sore throat, morning headache, difficulty concentrating, and mood changes. While obstructive sleep apnea can appear in every demographic, some factors increase an individual’s chance of developing the condition. Risk factors are excess weight or obesity, narrowed airway, high blood pressure, chronic nasal congestion, smoking, diabetes, gender (male), age (over 40), family history, and asthma. It is no surprise that as obesity rates continue to climb, so do cases of sleep apnea. Many mistake certain symptoms for other conditions, which contributes to the number of cases that go undiagnosed.
There are many reasons why the diagnosis of obstructive sleep apnea can be missed. For example, some people may not even be aware they have it because many telltale symptoms occur while asleep. So, the individual most likely does not remember waking several times throughout the night. Also, there may not be anyone to inform the individual of stalled breathing, gasping breaths, or loud snoring. Another reason is that sleep apnea is a progressive condition, meaning once symptoms develop, they can gradually worsen over time. Therefore, disrupted sleep becomes the “norm,” and it isn’t given much thought. Sleep apnea is also overlooked because symptoms that most people commonly experience in the daytime are similar to other conditions, both mental and physical, and can be incorrectly diagnosed as depression, anxiety, or even a common cold. Awareness and education about sleep apnea is surprisingly low, which contributes to untreated and undiagnosed cases. Without proper awareness of the condition, people may believe that they simply aren’t “good sleepers” and do not realize their symptoms could be something more serious that could lead to severe health complications. Finally, individuals may be aware of obstructive sleep apnea and may feel certain that they have it, but do not want to undergo rigorous testing or treatment for the condition. Luckily, the use of pulse oximetry has become more prevalent in screening for obstructive sleep apnea, saving many from the inconvenience of in-lab polysomnography, PSG, testing.
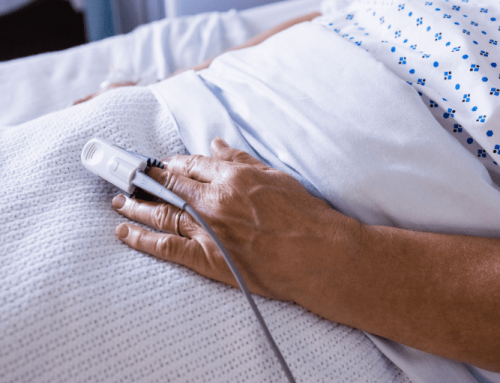
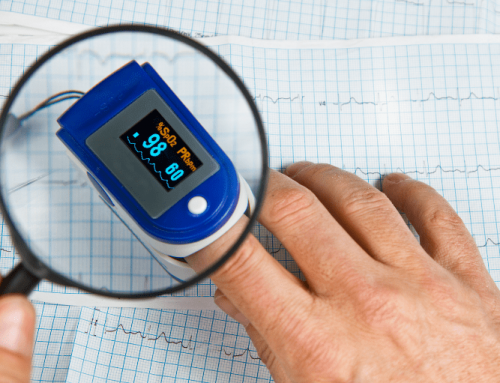
While polysomnography is still the most reliable test for the diagnosis of sleep apnea, it is time-consuming, expensive, and uncomfortable. PSG testing involves several monitors that measure heart, lung, and brain activity, as well as breathing patterns, arm and leg movements, and blood oxygen levels. However, pulse oximetry can be used to determine if a test like this is necessary or help assess the severity of obstructive sleep apnea. Overnight pulse oximetry is a simple test that can be done in the comfort of your own home. The test involves wearing a clip over a finger, held in place with a piece of tape. The clip connects to a small device that continuously records blood oxygen levels and heart rate throughout the night. The data is gathered into a graph, which will show if blood oxygen content drops at any time during the night. If this occurs more than five times per hour throughout the night, it could be a sign of sleep apnea.
Overnight pulse oximetry testing is simple and reliable, and does not require a change in routine, or sleeping in a strange environment. More importantly, it can give you the answers you need without having to spend an absurd amount of money. Overnight oximetry is useful in determining whether additional testing is required to adequately diagnose sleep apnea. It is also helpful to ensure current treatments, such as CPAP therapy or supplemental oxygen use, are effective at maintaining healthy blood oxygen levels. As the technology behind pulse oximetry continues to evolve and progress, its use is becoming more widespread. In fact, now, pulse oximetry is even being considered for general screening purposes. For individuals with underlying health conditions that could potentially lead to sleep apnea, like cardiovascular diseases, or individuals with several risk factors, may benefit from overnight oximetry even without showing typical symptoms. This is beneficial for early detection and possibly preventing other health complications. Certain lifestyle changes can help with improving sleep. However, sometimes medical intervention is necessary. If you believe you may be at risk for sleep apnea or have struggled with restless sleep, talk with your physician about Vitalistics’ overnight pulse oximetry testing. Don’t continue to suffer from poor sleep.